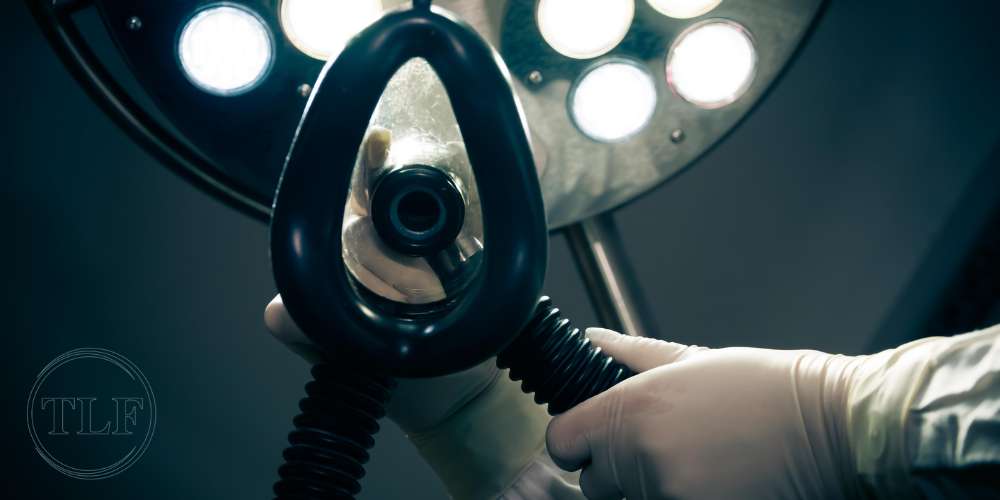
Anesthesia awareness, a rare but profoundly distressing phenomenon, occurs when a patient regains partial consciousness during surgery or medical procedures under general anesthesia. This condition exposes individuals to an awareness of their surroundings, potentially accompanied by pain and an inability to communicate due to the paralytic agents often used in anesthesia.
At TLF: The Medical Injury Law Firm, we understand the deep psychological and physical impact anesthesia awareness can have on patients. Our Ohio and Northern Kentucky anesthesia mistake attorneys provide compassionate legal representation to those who have endured this experience, ensuring they receive the recognition and compensation they deserve.
To learn more about this rare medical phenomenon and your legal rights following an anesthesia awareness experience, call TLF: The Medical Injury Law Firm at (800) 698-4054 to meet with a Northern Kentucky or Cincinnati medical malpractice attorney on our team today.
What is Anesthesia Awareness?
Anesthesia awareness, or intraoperative awareness, is a medical condition that occurs when a patient regains partial or full consciousness during a surgical procedure under general anesthesia without the ability to move or communicate distress to the medical team. This phenomenon can result in varying degrees of recall, from vague, dream-like experiences to clear and conscious recollections of the surgery, including sensations of pain, pressure, or emotional distress.
Levels of Consciousness Under Anesthesia
Anesthesia is designed to create a controlled and reversible state of unconsciousness, allowing for pain-free unawareness during surgical procedures. Levels of patient awareness can be managed by anesthesiologists using a combination of anesthetic drugs to achieve desired states, such as sedation, analgesia, and muscle relaxants.
In the section below, we’ll break down the various levels of awareness during anesthesia, highlighting the importance of precisely administering anesthesia to prevent intraoperative awareness during surgery.
Unconsciousness
Unconsciousness under anesthesia is a medically induced state where the patient completely lacks awareness and responsiveness to external stimulants, including pain. This level of anesthesia is achieved by administering a combination of medications, including sedatives, analgesics, and muscle relaxants, tailored to the individual’s needs and the specifics of the surgery.
The depth of unconsciousness is closely monitored by the anesthesia provider using sophisticated equipment for blood pressure and brain function monitoring, ensuring the patient remains in a stable and appropriate level of sedation throughout the procedure.
Sedation
Unlike deep unconsciousness, sedation can range from minimal, where the patient is relaxed but fully responsive, to deep, where they are on the edge of consciousness but can still be awakened with significant stimulation.
This versatility makes lighter anesthesia useful for procedures that do not require a full loss of consciousness or for patients for whom deep anesthesia may pose increased risks. An anesthesia provider should adjust the sedative dosages to match the patient’s needs, ensuring safety and comfort while maintaining vital functions and the ability to respond to verbal cues or physical stimulation.
Full Awareness
Full awareness under anesthesia occurs when a patient regains complete consciousness during a surgical procedure while still under the influence of anesthetic drugs. This means the patient can experience sensory input, including pain, and possess full memory of the events without the ability to move or communicate due to the muscle paralysis induced by general anesthesia.
Such instances of intraoperative awareness are deeply traumatic and can lead to long-lasting psychological consequences, including post-traumatic stress disorder (PTSD), severe anxiety, and fear of future medical treatments.

What Causes Anesthesia Awareness?
Anesthesia awareness occurs for many reasons, including variations in patients’ responses to anesthetic drugs, dosing miscalculations, equipment malfunctions, or the necessity for light anesthesia in high-risk surgeries to maintain cardiovascular stability.
Differences in metabolism and tolerance to anesthetics mean that some patients may metabolize these drugs faster than anticipated, emerging from their intended level of unconsciousness. Additionally, certain surgical situations, such as emergency procedures or operations on pregnant women, may require a lower dose, inadvertently leading to instances of anesthetic awareness.
Potential Risk Factors
Identifying potential risk factors for anesthesia awareness is crucial for minimizing its occurrence and ensuring patient safety. These can include the type of surgery, with cardiac surgery, trauma cases, and emergency procedures inherently requiring lighter levels of anesthesia to preserve vital functions, increasing the risk of awareness.
Patient-specific characteristics also play a significant role; for example, individuals with a history of substance abuse or chronic pain may have an altered response to anesthetic agents, necessitating changes in the anesthetic dose needed.
Additionally, the use of neuromuscular blocking drugs, which paralyze muscles without affecting consciousness, can predispose patients to awareness if the anesthetic depth is insufficient. Technological factors, such as the failure of anesthesia delivery equipment or inadequate monitoring of anesthetic depth, further contribute to the risk.
How Common is Anesthesia Awareness?
Anesthesia awareness remains relatively rare in modern anesthesia practice. Current estimates suggest that it occurs in approximately 0.1% to 0.2% of all surgical cases with patients undergoing general anesthesia, translating to roughly 1 to 2 cases per 1,000 procedures.
However, these statistics can vary depending on factors such as the type of surgery, patient population, and the definition used to classify awareness. Certain high-risk surgeries or patient populations may have a slightly higher incidence of awareness.
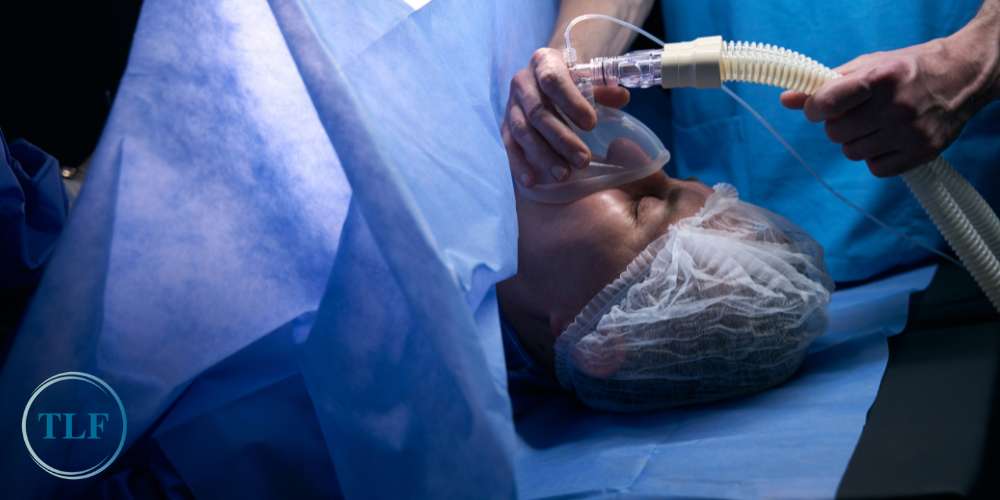
Signs and Symptoms of Anesthesia Awareness
Understanding the signs and symptoms of anesthesia awareness is important for both healthcare providers and patients. While rare, intraoperative awareness can have psychological and emotional repercussions for individuals who experience it.
Recognizing the subtle indicators of anesthesia awareness, such as recall of intraoperative events or sensations of pain, is essential for early detection and intervention.
Sensory Perceptions
Sensory perceptions during general anesthesia represent a complex interplay between the patient’s neurophysiological responses and the pharmacological effects of anesthetic agents. While the primary goal of anesthesia is to induce a state of unconsciousness, surgical patients may occasionally experience sensory phenomena despite being under general anesthesia.
These perceptions can manifest in various forms, including auditory sensations, tactile stimuli, or visual imagery, and may range from fleeting sensations to vivid and distressing experiences. Factors such as the depth of anesthesia, individual susceptibility, and the nature of the surgical procedure can influence the likelihood and intensity of sensory perceptions.
Feelings of Pressure or Pain
Feelings of pressure or pain during general anesthesia can be distressing for patients and present challenges for healthcare providers. Despite the intention to provide complete pain relief and unconsciousness during surgery, some individuals may experience sensations of pressure or discomfort.
These feelings of pressure or pain can arise from various factors, including inadequate anesthesia depth, individual variations in drug response, or using neuromuscular blocking agents that prevent movement but do not eliminate sensation.
Inability to Move or Communicate
The inability to move or communicate during general anesthesia is fundamental to ensuring patient safety and comfort during surgical procedures. While under the effects of general anesthesia, the anesthetized patient experiences temporary paralysis induced by neuromuscular blocking agents, which prevent voluntary muscle movement and vocalization.
This state of immobility and silence is essential for the surgical team to perform procedures without interference and for patients to remain still and avoid injury. However, it also means that patients may be unable to express discomfort or distress during surgery, making it challenging for healthcare providers to detect and address potential issues such as insufficient anesthesia or anesthesia awareness.
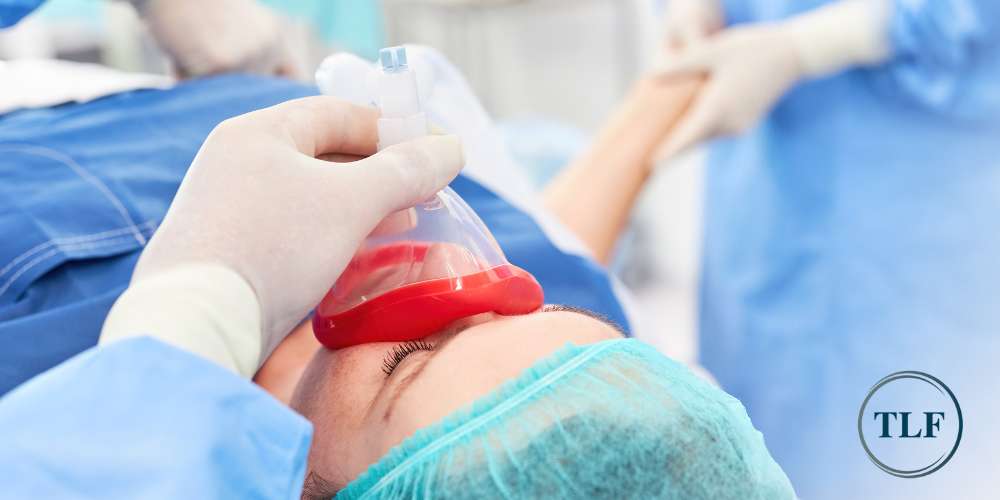
How To Prevent Anesthesia Awareness
Nurse anesthetists employ several strategies to minimize the risk of intraoperative awareness, starting with thorough preoperative assessments to evaluate each patient’s medical history, medication use, and individual response to general anesthesia.
Tailoring anesthesia protocols to the specific needs of the patient and the surgical procedure is crucial, ensuring that appropriate anesthetic agents and dosages are administered to achieve and maintain the desired level of unconsciousness.
Advanced monitoring technologies, such as bispectral index (BIS) monitoring and electroencephalography (EEG), help assess the depth of general anesthesia in real-time, allowing for prompt adjustments if necessary.
Consequences of Anesthesia Awareness
The consequences of anesthesia awareness can be profound and far-reaching. From a physical standpoint, individuals who experience anesthesia awareness may endure acute pain and discomfort during surgery, leading to postoperative complications such as increased stress response, delayed wound healing, and prolonged recovery times.
The psychological impact of anesthesia awareness can also be particularly distressing, often resulting in symptoms of post-traumatic stress disorder (PTSD), anxiety, sleep disturbances, depression, and persistent fear of medical procedures. This psychological impact can significantly impair a patient’s quality of life, affecting their ability to trust healthcare providers and undergo future surgeries.
Intraoperative awareness can also have broader implications for healthcare systems, leading to increased healthcare costs associated with prolonged hospital stays, additional medical interventions, and ongoing psychological support for those who have experienced anesthesia awareness.
What are My Legal Rights After Anesthesia Awareness?
If you’ve experienced anesthesia awareness, you have legal rights that may entitle you to compensation for the physical and psychological harm you’ve suffered. Anesthesia awareness can result from medical negligence or errors in anesthesia administration, and you may have grounds for a medical malpractice claim. Your rights include seeking damages for medical expenses, lost wages, emotional distress, and other losses and/or damages resulting from the incident.
To pursue legal action, you’ll need to consult with an experienced medical malpractice attorney. At TLF: The Medical Injury Law Firm, our attorneys regularly evaluate anesthesia awareness cases, collect evidence, and help clients through the legal process.

Why You Need an Experienced Medical Malpractice Attorney On Your Side
Medical malpractice claims are extremely complex, so working with an experienced medical negligence law firm is crucial. These attorneys possess the legal knowledge and resources to investigate your case, gather evidence, and build a strong argument on your behalf.
Experienced medical malpractice attorneys also have access to expert witnesses, such as anesthesiologists and medical professionals, who can provide beneficial testimony to support your claim. By partnering with a skilled attorney, you can level the playing field against insurance companies and healthcare providers, increasing your chances of securing the compensation you deserve due to anesthesia awareness.
Why Choose TLF: The Medical Injury Law Firm?
Choosing TLF: The Medical Injury Law Firm means partnering with a team of dedicated professionals with decades of experience handling medical malpractice cases, including those involving anesthesia awareness. TLF has a proven track record of success in advocating for the rights of individuals harmed by medical negligence. Our experienced attorneys have the resources and commitment to pursue justice for our clients, holding negligent healthcare providers accountable for their actions.
At TLF, we are passionate about fighting for the rights of those affected by anesthesia awareness and are dedicated to helping you secure the compensation you deserve.
Call an Experienced Anesthesia Awareness Attorney at TLF For a Free Consultation
The experienced anesthesia awareness attorneys at TLF are ready to listen to your story, answer your questions, and provide you with the guidance and support you need. We understand the challenges you’re facing, and we’re here to fight for your rights and pursue the justice you deserve.
Contact TLF: The Medical Injury Law Firm by calling (800) 698-4054 or send us a message online to schedule your free consultation today.